October 2021
Inside This Issue
Interoperability Requirements:
The October edition of Perspectives has yet another update on interoperability requirements. You may remember that in April the requirement was introduced at IM.02.02.07 with five elements of performance. Then in May, EP 5 was edited to make it clearer that the automated notice you must send when a patient is admitted or receives services in your emergency room needs to go to the patient’s primary care (or other) practitioner/group and applicable post-acute care services providers/suppliers.
As of October, there is yet one more change now at RI.01.02.01, EP 1 along with a new note 1 explaining this automated notice requirement from a patient rights perspective. Be particularly careful in reading this change in Perspectives and be sure to use their link to the prepublication page. While Note 1 is displayed in Perspectives, the change to EP 1 itself it not displayed in the Perspectives article.
The EP makes it clear that notice should be sent for admissions, discharges, and transfers out of the hospital. TJC also mentions the patient’s family in EP 1, however families are not likely to have an electronic infrastructure to receive such notices. The new note 1 states that the automated notice must be sent to “an established primary care practitioner, primary care practice group or entity, or other practitioner group or entity, as well as all applicable post-acute services providers and suppliers.”
In addition, the note states that the hospital must have a process for documenting a patient’s refusal to permit notification of registration to the emergency department, admission to an inpatient unit, or discharge or transfer from the emergency department or inpatient unit.”
We believe that this will mean hospitals will need to promptly inform patients who present to your emergency department services or inpatient admission that their primary care providers and service providers are going to be notified of the service unless the patient requests that such automated notice be stopped. We would anticipate that most patients will not object to this notice, but there will be exceptions and in these cases the patient’s wishes must be honored.
While earlier iterations of this requirement focused on creating the electronic infrastructure capacity to send the notice, this means you also need a process to identify those who object, and to electronically cut off such notice before it is sent. There are already many such notices of rights and responsibilities already placed in front of patients for signature upon arrival in the hospital and you may have to expand one of the existing forms to add information about this automated notice.
While the full scope of this electronic notice process is becoming clearer, we think hospitals must act now to identify a specific department or designated staff who will be responsible for informing the patient of these notification requirements and obtain their authorization, or, if the patient objects, manage the process to cancel the automatic electronic notification.
These requirements are already applicable in hospitals that use Joint Commission for deemed status, and become applicable in those hospitals that do not have a deeming relationship with TJC as of April 1, 2022.
We have not seen this issue yet scored by TJC, although that may be because many hospitals are still building this evolving capacity, but please let us know if you become one of the early victims of the evolving process.
Psychiatric Patient Boarding in the ED: 
The October Perspectives also discusses an edition of Quick Safety that TJC had published in July discussing Boarding of Psychiatric Patients in the Emergency Room. There is advice from TJC in three areas: addressing patient needs, supporting ED staff, and improving the environment. The advice seems sound, but off target on the root causes we hear hospitals citing when exploring the reasons why there is boarding of psychiatric patients and the actions that the health care system has to take to improve the situation.
Nutritional Assessments:
This month’s Consistent Interpretation column discusses two elements of performance under PC.01.02.01 relative to nutritional assessments and one EP from PC.01.03.01. The first EP discussed in the article is PC.01.02.01, EP 2 which states that the hospital defines in writing criteria that identify when additional, specialized, or more in-depth assessments are performed. This was only scored in less than 2% of hospital surveys last year. Starting with EP 2 is somewhat like starting in the middle of a story.
We believe you should also look at EP 1, which is really the starting point in this discussion. EP 1 requires the hospital to “define in writing the content of the screening, assessment and reassessment. The screening is the basic information gathered, often by nursing staff at the time of admission and based upon the information provided, it may result in a referral to a registered dietitian to perform a more in-depth assessment. We should also mention that TJC has an FAQ posted in the PC chapter discussing this issue that makes it clear that not every patient is required to have these screenings; the hospital gets to define when it is needed.
EP 2 requires the hospital to define criteria within that screening response that would trigger a referral for a more in-depth assessment. CMS provides additional guidance in their interpretive guidelines under tag A-0629 which requires this nutritional screen for all inpatients and outpatients whose stay is sufficiently long that they must be fed. In other words, you could choose to target your screening process on inpatients and in rare circumstances some outpatients as opposed to all inpatients and all outpatients. EP 2 would only be scored if the organization had failed to define when such a referral would be warranted.
The consistent interpretation column next discussed EP 3 which is scored very infrequently, on less than 1% of hospital surveys last year. This EP requires the hospital to define criteria that identify when nutritional plans are to be developed.
Lastly, the column discusses PC.01.03.01, EP 1 which the hospital to plan the patients care, treatment, and services based on the needs identified by the assessment, reassessment, and results of diagnostic testing. Here the scoring is much more significant, with this EP being scored in 31% of hospitals surveyed last year, however this EP is much broader in scope than just nutritional issues.
As you know TJC and CMS have had a significant focus on care planning and “gotchas” for failure to identify some comorbidity or new problem on the care plan. This could be a nutritional issue or just about any other care issue that led to this rate of scoring. It is our perception that only a small percentage of total scoring related directly to nutritional care planning.
EOP vs COOP:
While neither this month’s Perspectives or EC News has new requirements you need to prepare for, EC News does have several very useful articles on existing requirements that pose difficulty for hospitals.
The first of these is the October EC News article on Planning for Continuity of Operations. EM.02.01.01 requires a hospital to have an emergency operations plan, and EP 12 under this standard requires a continuity of operations strategy which covers two functions: succession planning and a delegation of authority plan.
This is one of the more frequently scored issues in the entire EM chapter as many organizations have failed to create such a COOP plan. Just about every hospital we see has an EOP, but unfortunately some fail to develop the COOP requirement either because of a lack of understanding or unwillingness to discuss succession planning.
This EC News article does an excellent job of differentiating between what an EOP is and what a COOP is, and they also help to focus on what a COOP really requires.
The key rationale behind the COOP is that key leaders may not be present during an emergency because in some fashion the emergency situation has cut them off from being present at the hospital. Thus, there should be delegation of authority plans for other leaders to take their place in managing the organization and the emergency.
This article should be shared with your team responsible for EM planning to help further refine your COOP, or to ensure that the COOP requirements are addressed.
Home Care – Most Frequently Cited EC, LS, and EM:
EC News quite frequently discusses the most frequently scored EC, LS and EM standards for hospitals, and this month they identify the most frequently scored in the home care program. Home care accreditation includes the hospice setting, which can include a 24-hour care setting which creates some similarity in findings to the hospital setting.
This article includes a top ten listing of standards scored most frequently and a top five listing of EPs scored the most frequently within those standards. As each standard has many elements of performance, the listing of EPs scored is particularly important to zeroing in on the core defect cited. The top five EPs are as follows:
- 02.01.30, EP 19: Smoke barriers are complete without penetrations (21.21%)
- 02.01.35, EP 10: Travel distance, weight and height of fire extinguishers (15.15%)
- 02.06.01, EP 14: Hospice hot water supply and temperature regulation (14.29%)
- 03.01.03, EP 20: EM plan test annually (13.40%)
- 02.01.01, EP 4: Safe storage of medical gases (11.80%)
The authors also provide some insight and guidance preventing some of these common EC, LS, EM findings in the home care accreditation program setting.
Preventing Eye and Skin Injuries:
The October issue of EC News has yet again, another good review article on preventing eye or skin injuries from corrosive chemicals, and the safety measures required for eye wash stations and other PPE. EC News and our Patton Post have discussed the need for eyewash stations where corrosive chemicals are used many times.
Yet the standard for some deficiency in the design, use, or maintenance of the eyewash station remains very frequently scored. This would indicate that there remain some knowledge deficits in when these stations are required and how to maintain them.
As cases in point, at different organizations we recently saw: an eyewash with an infrared triggering valve that required precise hand placement to initiate the water flow, and on top of that, it was tied to a timer that quickly shut off the continued flow if your hands moved away from the infrared beam.
Another required multiple manipulations to turn a sink faucet into an eyewash, combined with a paper towel dispenser that would prevent a user from being able to place their eyes over the eyewash because it blocked the placement of their head. This same eyewash was tested every week as required, but no one had considered the overall functionality of the eyewash. More recently we saw new construction with the area eyewash behind a locked door.
Clearly, greater insight is needed into the design, placement and functioning of these required safety devices. This EC News article is nice because it is not just designed for physical plant staff. It is written in a clear, concise, and explanatory manner that would be useful for clinical staff. Our suggestion is to share this summary article with clinical managers and then to ask if they have corrosive chemicals, and if so, is the eyewash properly designed, properly located, and functional for staff to use.
Compressed Gas Policies:
Proper storage of compressed gases in healthcare organizations remains a common challenge and this month’s EC News includes a checklist for policies compliant with both EC.02.05.09 and NFPA 99-2012 requirements. The checklist is located in this edition of EC News, and they also provide a link to access a Word version of the checklist for use within your organization. As issues with compressed gas storage are frequently cited, we would encourage our readers to download and use this document to help evaluate your policies and practices for gas storage.
Surveyors in Multi-Tenant Buildings:
The last page of the October EC News has an article, somewhat like an FAQ answering a frequently asked question, wondering where surveyors will look when surveying space operated by the accredited organization, within a building that has many tenants. The TJC response is that surveyors will look at the following. Unfortunately, the rationale or “the why” is not explained.
- The means of egress and any fire safety features for use by the public and inspect fire barriers on both sides if there is a difference in occupancy type. TJC provides an example of an accredited space identified as a business occupancy and on the other side an ambulatory or healthcare occupancy where they would want to look at both sides of the fire barrier.
- If the accredited space is on the ground floor of a multistoried building, then TJC would not examine stairways above the accredited space, however they would look to verify the stairwell does not include combustible storage or the exit from the stairwell is not blocked by some storage.
- If the accredited space is on an upper floor of a multistory/multitenant building the survey would include the stairways serving the upper floors as well as the exit path from the building.
- If the building contains a maintenance shop or basic boiler room not in the accredited space, TJC would not review it. However, if the room has a fully functional HVAC system that supports the accredited space, then they would review it.
- Not included in the article but worth reviewing again is the FAQ requiring life safety drawings in business occupancies. This has come as a bit of a surprise for some readers.
Pregnant Patients in the ED: 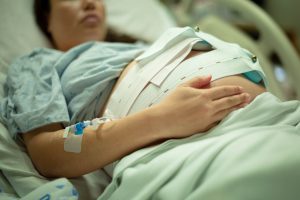
On September 17, CMS posted QSO 21-22 restating/reinforcing existing requirements for hospitals to provide care to pregnant patients presenting to the emergency room under EMTALA regulations. This memo is somewhat of a primer or refresher on EMTALA that looks to be useful to emergency room staff and physicians to remind them of existing obligations. The memo summarizes the three obligations under EMTALA as the:
- Screening requirement to determine if an emergency medical condition (EMC) exists
- Stabilizing requirement if an EMC exists and stabilization treatment is within the capability of the hospital
- Transfer requirement once the patient is stabilized or if a provider certifies the benefits of transfer outweigh the risks
Because of the severity of potential findings should CMS determine that EMTALA expectations have been violated, we would encourage our readers to circulate this memo to all emergency room staff and providers. If existing training does not already exist at your organization on EMTALA you might want to consider incorporation of this guidance into a training program. We also identified that CMS has an online training program for its surveyors that might be useful to staff at your hospital.
Maternal Morbidity:
The Agency for Healthcare Research and Quality issued a monograph this past month on the Contribution of Diagnostic Errors to Maternal Morbidity and Mortality. As TJC has new standards that are starting to be reviewed on maternal hemorrhage and pre-eclampsia we thought this work might be interesting to our readers. The document can be downloaded here.
Sterile Compounding in the Pharmacy:
Back in 2016 the Food and Drug Administration had issued draft guidance to the hospital industry relative to sterile compounding of pharmaceuticals addressing under what circumstances the FDA might want to examine the process and when they would not. That guidance has remained in draft status since 2016.
When published, the 2016 draft included advice that the FDA would not routinely inspect hospital pharmacy sterile compounding if these products were only distributed to patient care settings within one mile of the hospital pharmacy. That one mile limitation was concerning to hospitals as with mergers and acquisitions many multisite hospitals were separated by more than one mile.
At the beginning of October, the FDA revised its document and again issued it in draft status, but this time the one-mile limitation has been removed.
The FDA also issued guidance on under what general conditions they would not likely want to investigate. Those conditions include:
- The compounded drug products are administered only to patients within the hospital or health system.
- The compounded drug products are used or discarded within 24 hours of transfer out of the pharmacy.
- The drug products are compounded in accordance with all other applicable requirements of the FD&C Act and FDA regulations (e.g., the drug products are not made under insanitary conditions (section 501(a)(2)(A)) or misbranded (e.g., section 502(g)).
We know that many large hospitals have extensive sterile compounding and batch preparation activities and we would encourage our readers to review the entire FDA document. The document can be obtained from: https://www.fda.gov/media/97353/download
Consultant Corner
Dear Readers,
We are officially in the 4th quarter – before we know it, it’s going to be the New Year! If you are due for survey (or past due), please contact us soon to schedule your mock survey for 2022. We look forward to hearing from you!
Jennifer Cowel, RN MHSA
JenCowel@PattonHC.com
Kurt Patton, MS RPh
Kurt@PattonHC.com
John Rosing, MHA
JohnRosing@PattonHC.com
Mary Cesare-Murphy, PhD
MCM@PattonHC.com
